Thyroid & Infertility
Infertility can be a challenging and emotional journey, affecting many aspects of life. One crucial but often overlooked aspect of female infertility is the role of thyroid function. Thyroid disorders can significantly impact fertility, making it essential to understand and address these issues for those trying to conceive. In this blog, we will explore how thyroid disorders affect fertility and what can be done to manage these conditions effectively.
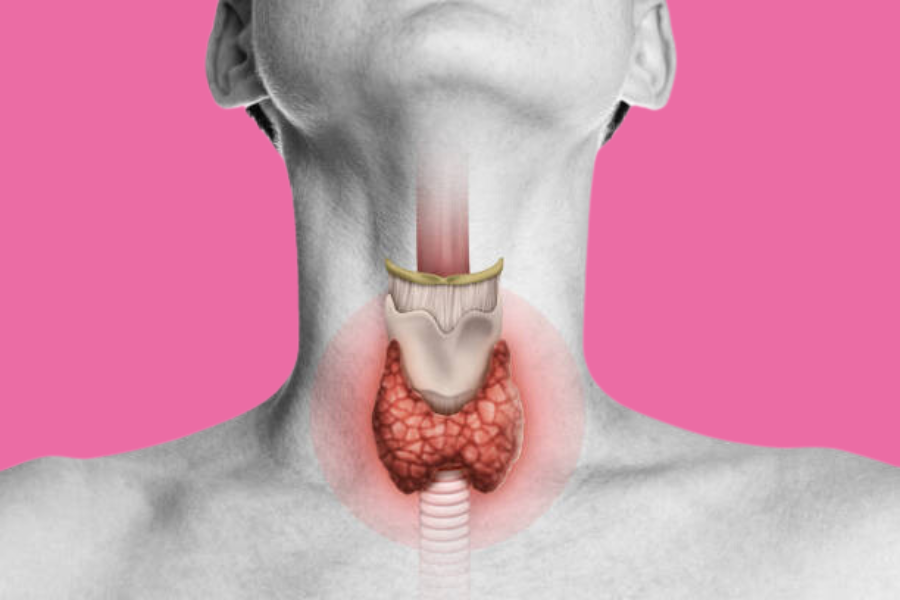
What is Thyroid?
The thyroid is a small, butterfly-shaped gland located at the base of the neck. Despite its small size, it plays a significant role in regulating various bodily functions by producing hormones that control metabolism, energy levels, and overall hormonal balance. The two primary hormones produced by the thyroid are thyroxine (T4) and triiodothyronine (T3), which influence the function of every cell, tissue, and organ in the body.
The Connection between Thyroid & Infertility
How Thyroid affect fertility?
- Hypothyroidism: It occurs when the thyroid gland does not produce enough thyroid hormones. Symptoms of hypothyroidism include fatigue, weight gain, depression, and irregular menstrual cycles. In terms of fertility, hypothyroidism can cause:
- Irregular menstrual cycles: This can make it difficult to predict ovulation.
- Anovulation: Absence of ovulation, leading to infertility.
- Increased risk of miscarriage: Due to hormonal imbalances.
- Luteal phase defect: Shortening of the second half of the menstrual cycle, affecting implantation.
- Hyperthyroidism: It occurs when the thyroid gland produces too much thyroid hormone. Symptoms include weight loss, anxiety, tremors, and irregular menstrual cycles. In terms of fertility, hyperthyroidism can cause:
- Irregular menstrual cycles: Similar to hypothyroidism, making ovulation unpredictable.
- Decreased ovarian reserve: Reduced number of viable eggs.
- Increased risk of premature birth: And low birth weight in pregnancies.
- Autoimmune thyroid disorders: Autoimmune disorders such as Hashimoto’s thyroiditis (leading to hypothyroidism) and Graves’ disease (leading to hyperthyroidism) can also affect fertility. These conditions interfere with the immune system’s ability to support a healthy pregnancy.
Diagnosis of Thyroid-Related Infertility
Diagnosing thyroid-related infertility is a comprehensive process that involves multiple steps to accurately identify and understand the nature of the thyroid disorder and its impact on fertility. Here’s an overview of the key diagnostic procedures:
1. Initial consultation
The diagnostic journey begins with an initial consultation. During this visit, your healthcare provider will:
- Conduct a thorough review of your medical history.
- Discuss your symptoms and any concerns you may have.
- Ask about your menstrual cycle regularity, duration, and any noticeable changes.
- Inquire about previous pregnancies, miscarriages, and overall reproductive health.
2. Physical examination
A physical examination may be performed to look for signs of thyroid dysfunction, such as:
- Enlargement or swelling in the neck (indicative of goitre).
- Dry skin, hair loss, and changes in weight (common in thyroid disorders).
- Reflexes and heart rate abnormalities.
3. Blood tests
Blood tests are essential to measure thyroid hormone levels and other related markers. These tests typically include:
- Thyroid-Stimulating Hormone (TSH): High TSH levels suggest hypothyroidism, while low TSH levels indicate hyperthyroidism.
- Free Thyroxine (FT4) and Free Triiodothyronine (FT3): These tests measure the active thyroid hormones in your blood. Low levels indicate hypothyroidism, and high levels suggest hyperthyroidism.
- Thyroid Antibodies: Tests for thyroid peroxidase antibodies (TPOAb) and thyroglobulin antibodies (TgAb) help diagnose autoimmune thyroid disorders like Hashimoto’s thyroiditis and Graves’ disease.
4. Imaging tests
Imaging studies provide a visual assessment of the thyroid gland’s structure and any abnormalities. Common imaging tests include:
-
- Thyroid ultrasound: Uses sound waves to create an image of the thyroid gland, helping detect nodules, cysts, and gland enlargement.
- Radioactive Iodine Uptake test (RAIU): Measures the thyroid gland’s ability to absorb iodine, which is crucial for hormone production. This test helps differentiate between different types of hyperthyroidism.
5. Additional Diagnostic Procedures
Depending on your individual case, your healthcare provider may recommend additional tests, such as:
-
- Fine-needle aspiration biopsy: In cases where nodules are detected, a biopsy may be performed to rule out thyroid cancer.
- Basal body temperature charting: Monitoring basal body temperature can help identify ovulation patterns and any disruptions caused by thyroid dysfunction.
6. Hormonal Evaluation
Since thyroid disorders can affect overall hormonal balance, your healthcare provider may also assess other hormones involved in reproduction, such as:
-
- Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH): To evaluate ovarian function.
- Prolactin: Elevated levels can interfere with ovulation and are sometimes associated with hypothyroidism.
- Estradiol and Progesterone: To assess ovarian and luteal phase function.
7. Comprehensive Fertility Assessment
In addition to thyroid function tests, a comprehensive fertility assessment may be performed to evaluate other factors that could affect your ability to conceive. This includes:
-
- Hysterosalpingography (HSG): An X-ray test to check for blockages in the fallopian tubes.
- Transvaginal ultrasound: To assess the ovaries, uterus, and endometrial lining.
- Semen analysis: To evaluate the male partner’s fertility.
By combining these diagnostic approaches, healthcare providers can develop a thorough understanding of how thyroid disorders are affecting your fertility. This comprehensive evaluation is essential for creating an effective treatment plan tailored to your specific needs, ultimately improving your chances of conceiving.
Treatment of Thyroid-Related Infertility
Treating thyroid-related infertility involves addressing the underlying thyroid disorder to restore hormonal balance and improve reproductive health. The treatment plan will depend on whether you have hypothyroidism, hyperthyroidism, or an autoimmune thyroid condition. Here’s a detailed overview of the treatment options:
Hypothyroidism Treatment
Hypothyroidism is characterized by an underactive thyroid gland that produces insufficient thyroid hormones. Treatment focuses on hormone replacement and lifestyle adjustments:
- Medication
- Levothyroxine: This synthetic thyroid hormone is the standard treatment for hypothyroidism. It helps restore normal hormone levels, thereby regulating metabolism and supporting normal ovulation and menstrual cycles.
- Dosage monitoring: Regular blood tests are essential to monitor TSH levels and adjust the medication dosage to ensure optimal thyroid function.
-
Diet and Lifestyle
- Balanced diet: A diet rich in iodine, selenium, and zinc can support thyroid health. Foods such as fish, dairy, eggs, nuts, and seeds are beneficial.
- Exercise: Regular physical activity helps maintain a healthy weight and overall well-being, which can positively impact thyroid function and fertility.
Hyperthyroidism Treatment
Hyperthyroidism occurs when the thyroid gland produces excessive thyroid hormones. Treatment aims to reduce hormone production and alleviate symptoms:
-
Medication
- Antithyroid drugs: Medications like methimazole and propylthiouracil (PTU) help reduce thyroid hormone production. These drugs are typically the first line of treatment for hyperthyroidism.
- Beta-blockers: These may be prescribed to manage symptoms such as rapid heart rate and anxiety until thyroid hormone levels are under control.
-
Radioactive Iodine Therapy
- Purpose: This treatment involves taking radioactive iodine orally. The iodine is absorbed by the thyroid gland, where it gradually destroys overactive thyroid cells, reducing hormone production.
- Monitoring: Patients need regular follow-ups to monitor thyroid function post-treatment, as this therapy can sometimes lead to hypothyroidism, requiring subsequent hormone replacement therapy.
-
Surgery
- Thyroidectomy: In cases where medication and radioactive iodine therapy are not effective or suitable, surgical removal of part or all of the thyroid gland may be necessary. Post-surgery, patients will require lifelong thyroid hormone replacement therapy.
Treatment of Autoimmune Thyroid disorders
Autoimmune thyroid conditions, such as Hashimoto’s thyroiditis and Graves’ disease, require specific treatments to manage both the thyroid disorder and its impact on fertility:
-
Immunosuppressive therapy
- For autoimmune conditions, immunosuppressive drugs may be used to reduce the immune system’s attack on the thyroid gland.
- For autoimmune conditions, immunosuppressive drugs may be used to reduce the immune system’s attack on the thyroid gland.
-
Hormone Replacement and Regulation
- Hashimoto’s Thyroiditis: Typically treated with levothyroxine to manage hypothyroidism.
- Graves’ Disease: Managed with antithyroid medications, radioactive iodine, or surgery, similar to other hyperthyroidism treatments.
Assisted Reproductive Technologies (ART)
For couples struggling with thyroid-related infertility, Assisted Reproductive Technologies (ART) can be an effective solution when combined with thyroid management:
-
In Vitro Fertilization (IVF)
- IVF involves fertilizing an egg with sperm outside the body and then implanting the embryo into the uterus. Properly managing thyroid levels can enhance the success rate of IVF by creating a favourable environment for implantation and pregnancy.
- IVF involves fertilizing an egg with sperm outside the body and then implanting the embryo into the uterus. Properly managing thyroid levels can enhance the success rate of IVF by creating a favourable environment for implantation and pregnancy.
-
Ovulation Induction
- Medications like clomiphene citrate or gonadotropins may be used to stimulate ovulation in women with thyroid-related anovulation (absence of ovulation).
- Medications like clomiphene citrate or gonadotropins may be used to stimulate ovulation in women with thyroid-related anovulation (absence of ovulation).
-
Intracytoplasmic Sperm Injection (ICSI)
- In cases where male factor infertility is also present, ICSI can be used in conjunction with IVF to inject a single sperm directly into the egg.
Why choose Shukan Hospital & IVF Centre in Ahmedabad for Thyroid-Related Infertility treatment?
- Custom treatment plans for thyroid-related infertility.
- Collaboration between endocrinologists, gynecologists, and fertility specialists.
- State-of-the-art diagnostics and treatments.
- Care from consultation to post-treatment.
- Positive outcomes from managing thyroid-related infertility.
FAqs
How long does it take to treat thyroid-related infertility?
The duration of treatment varies depending on the specific thyroid disorder and individual response to treatment. Regular monitoring and adjustments are essential for effective management.
Can thyroid disorders cause irregular periods?
Yes, thyroid disorders, whether hypothyroidism or hyperthyroidism, can disrupt the menstrual cycle. Irregular periods can affect ovulation and, consequently, fertility.
How do thyroid disorders affect the timing of ovulation?
Thyroid hormones play a role in regulating the menstrual cycle and ovulation. Both hypothyroidism and hyperthyroidism can lead to irregular or absent ovulation, making conception more difficult.
Are thyroid disorders hereditary?
Thyroid disorders can have a genetic component. If there is a family history of thyroid conditions, the risk of developing a thyroid disorder may be higher.
How long does it take to see improvement after starting thyroid treatment?
The timeline for seeing improvement can vary depending on the type of thyroid disorder and the response to treatment. Some individuals may experience relief from symptoms and hormonal balance within a few weeks, while others may take longer.
Can thyroid disorders affect egg quality?
Yes, thyroid disorders can impact ovarian function and the quality of eggs. Hypothyroidism, in particular, can affect hormonal balance and contribute to reduced ovarian reserve, which may affect egg quality.
Can thyroid disorders cause pregnancy complications?
Yes, thyroid disorders can increase the risk of pregnancy complications, including miscarriage, preterm birth, and low birth weight. Proper thyroid management during pregnancy is essential for a healthy outcome.
What are the potential effects of thyroid treatment on my menstrual cycle?
Proper thyroid treatment can help regulate menstrual cycles and improve ovulation. Hormone levels should stabilize, leading to more predictable and regular periods.
Can lifestyle changes help improve thyroid function and fertility?
Yes, lifestyle changes such as maintaining a balanced diet, regular exercise, stress management, and adequate sleep can support overall thyroid health and enhance fertility.
How often should I have my thyroid levels checked while undergoing infertility treatment?
Monitoring thyroid levels is essential while undergoing infertility treatment. Regular blood tests can help ensure that hormone levels are stable and treatment adjustments are made as needed.
Meet Our Specialists

Dr. Prakash Patel
MBBS, DGO, Diploma in Laparoscopy, Diploma in Fetal Medicine
Specialities: IVF, Male Infertility, Female Infertility
Experience: 10+ years
Language: English, Hindi, Gujarati
- Expert in advanced laparoscopic surgeries.
- Successfully manages complex IVF cases and recurrent miscarriages.
- Proficient in high-risk pregnancy and advanced IVF treatments.
- Compassionate, personalized patient care.
- Certified by top institutions in France and Croatia.
- Member of FOGSI and ISAR, recognized internationally.

Dr. Ajay Prajapati
MBBS (Bachelor of Medicine, Bachelor of Surgery), MS (Master of Surgery)
Specialities: IVF, Infertility, Fetal medicine
Experience: 10+ years
Language: English, Hindi, Gujarati
- Over a decade of hands-on experience in fertility and pregnancy challenges.
- Expert in advanced laparoscopy for minimally invasive surgeries.
- FOGSI-certified sonologist, ensuring accurate pregnancy assessments.
- Known for successful outcomes and trusted care in high-risk cases.
- Earned patient trust across Gujarat and beyond
Blogs related to Female Infertility
What is the difference between IVF & Test tube baby?
In the world of fertility treatments, you often hear terms like "IVF" and "test tube baby" used interchangeably. This can create confusion for...
IVF after miscarriage: What you need to know
Experiencing a miscarriage can be a profoundly emotional and challenging time. For many, the journey toward parenthood does not end with a...
The Climate Connection: Weather’s Impact on IVF Success Rates
In vitro fertilization (IVF) is a highly controlled medical process, but can external factors like weather influence its success? This blog explores...
The Human Touch: Emotional and Ethical Considerations in IVF
In vitro fertilization (IVF) is more than a complex medical procedure; it represents a profound journey of hope, emotions, and critical ethical...
Modernizing the IVF Lab: Overcoming Challenges with New Innovations
In vitro fertilization (IVF) has transformed reproductive medicine, offering hope to individuals and couples facing infertility. At the core of this...
The role of Preimplantation Genetic Testing (PGT) in IVF: benefits & considerations
At Shukan Hospital & IVF Centre, we are at the forefront of advanced fertility treatments, striving to provide our patients with the best...
IVF vs. IUI: Which fertility treatment is right for you?
Navigating the path to parenthood can be both exciting and daunting, especially when facing fertility challenges. For many individuals and couples,...
5 Best IVF hospitals in Ahmedabad
Choosing the right IVF hospital is a crucial step in the journey towards parenthood, especially in a city as vibrant as Ahmedabad. With advancements...
Key Questions Every Pregnant Woman Needs to Ask Their Gynecologist
Pregnancy is an exciting journey filled with anticipation, but it can also be a time of uncertainty and questions. It's essential to have open and...
IVF Embryo Grading and Success Rates
IVF (In Vitro Fertilization) has become a beacon of hope for many couples struggling with infertility. One of the critical steps in the IVF process...
Fertility Treatments for Women with Low AMH and Regular Periods
Understanding Low AMH Anti-Müllerian Hormone (AMH) is produced by the small follicles in a woman's ovaries and serves as a marker of ovarian...
The Role of Genetics in Female Infertility
Infertility is a complex and often emotionally challenging issue that affects millions of women worldwide. Understanding the underlying causes is...
How to Prepare for Fertility Treatments: A Comprehensive Guide
Embarking on the journey of fertility treatments is a significant step towards achieving your dream of parenthood. Proper preparation can greatly...
Comprehensive Care Post IVF Transfer
The journey through In Vitro Fertilization (IVF) is both challenging and rewarding. After the embryo transfer, a critical phase begins that requires...
Scientific way to understand IVF for Infertile Patients
Introduction:Infertility can be a challenging and emotional journey for individuals and couples dreaming of starting a family. In recent years,...
Unlocking the Secrets: Epigenetics at the Core of Embryonic Development
Embarking on the extraordinary journey of embryonic development, Shukan Hospital and IVF Center stand as pillars of expertise, guiding aspiring...
Why Blastocyst Transfer for Healthy Pregnancy
Introduction:Blastocyst embryo transfer is a technique used in assisted reproductive technologies (ART), The method of transferring embryos during...
NAVIGATING THE JOURNEY ,UNDERSTANDING EMBRYO CULTURE CONDITION IN IVF LABS FROM A PATIENTS PERSPECTIVE.
Introduction:The IVF lab plays a central and pivotal role in the development of embryos during the in vitro fertilization (IVF) process. Embryo...
Demystifying Common Infertility Myths: Separating Fact from Fiction
Infertility is a condition that affects many couples who are trying to conceive a child. It is defined as the inability to get pregnant after one...
Struggling with poor ovarian reserve! Know All about it and it’s treatment!
Ovarian reserve (POR) is a condition in which the number of eggs in a woman's ovaries is less than would be expected for her age. As it can affect...
Myths and Facts About IVF
While in-vitro fertilization (IVF) is becoming increasingly popular as an effective infertility treatment, there are still some myths associated...
The Importance of Mental and Emotional Health During the Fertility Journey
During fertility treatments, the body goes through a lot, which can also impact the mind. When individuals choose to undergo in vitro fertilization...
Why India is the Best option for IVF treatment?
In vitro fertilization (IVF) treatments are popular in India due to their lower costs and high success rates. Further, India is home to some of the...
Why are my Fertility Treatments ending up in failed cycles?
Fertility treatments that are not successful can take a toll on the couple, both emotionally and financially. However, the one benefit is that...
Why IVF fails. ?
According to the latest statistics from the Society for Assisted Reproductive Technologies (www.sart.org) in the year 2011, there were a total of...
Why Male and Female infertility is increasing nowadays?
Male and female infertility is caused by certain medical issues that prevent them from becoming pregnant. India has an alarming increase in...
How to choose right IVF clinic?
Top 10 tips while choosing the right IVF clinic for youIf you're considering going to a fertility clinic as your next step, do some research before...